Case Studies

From Chaos to Clarity: A 60-Day Workflow Rebuild That Boosted Collections by 40%
The Challenge
This multi-practice group was experiencing a compounding set of financial and operational challenges that many practices quietly struggle with. Eligibility denials were climbing due to inconsistent verification, incomplete benefit checks, and unclear PA requirements, leaving front-desk staff without a reliable workflow. Their third-party vendor provided little transparency and allowed A/R to age out with minimal follow-up, while manual data entry errors created constant rejections, rework, and delays. Claims routinely stalled without clear ownership, cash flow became unpredictable, and leadership struggled to identify where revenue was leaking or how to correct it—resulting in a reactive, overloaded billing cycle with mounting A/R and preventable losses.
Key Issues:
Massive eligibility denials due to inaccurate or incomplete verification
No structured workflow for benefits verification or prior authorizations
Third-party vendor allowing A/R to age out with limited follow-up
Manual data entry leading to high error rates and preventable rejections
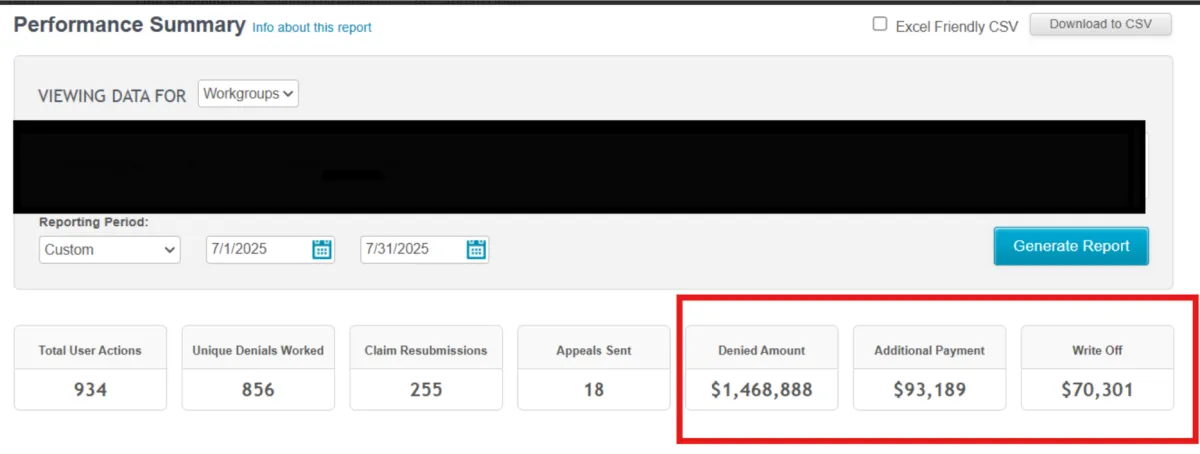
🟥 Starting Point: $1.4M in denied claims
The Solution
The practice required more than surface-level fixes — it required a complete rebuild of its front-end processes, A/R workflows,
and operational visibility. We stepped in with a structured, hands-on approach designed to eliminate preventable denials,
restore accountability, and create sustainable billing operations. Our methodology focused on simplifying complex tasks for
staff, introducing tracking systems where none existed, and replacing reactive processes with proactive, predictable
workflows.
Key Changes and Optimizations:
Implemented a simplified verification SOP for non-medical staff to prevent avoidable eligibility and COB denials.
Built a full PA tracking system with automated reminders for approvals, expirations, and renewals.
Reorganized the A/R worklist to support priority-based follow-up, timely filing compliance, and clearer task ownership.
Completed a 45-day A/R cleanup, targeting aged claims, stale denials, and ignored vendor handoffs.
Delivered staff training on eligibility, documentation accuracy, and intake workflows to eliminate preventable rework.
The Results (Within The First 60 Days)
The improvements were immediate and measurable. By addressing the root causes of denials, tightening front-end
accuracy, and restoring structure to the A/R cycle, the practice saw a dramatic turnaround in both financial performance
and operational efficiency. What had once been a reactive, error-prone billing environment became a streamlined,
accountable workflow with predictable cash flow and far fewer surprises. Within the first 60 days, the practice achieved:
Eligibility denials dropped 72%
A/R over 90 days reduced 55%
Clean claim rate increased to 98.3%
Patient collections increased 40%
Front desk accuracy improved 68%
Claims no longer sit in the worklist beyond 7–10 days
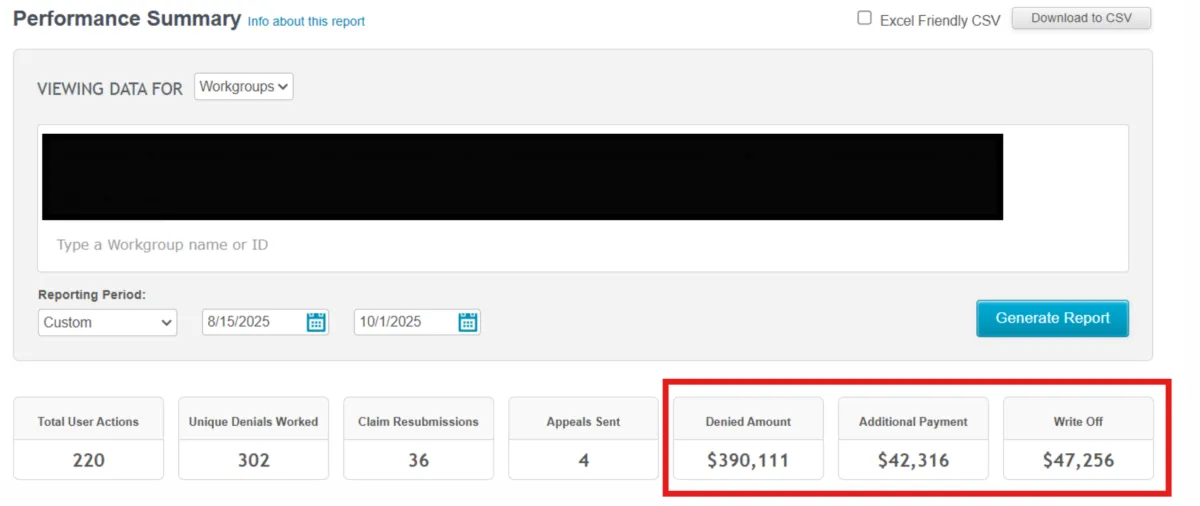
🟩AFTER 60 DAYS: $1.1 IN RECOVERED REVENUE
The Takeaway
This 60-day transformation shows what can happen when preventable denials, outdated workflows, and vendor blind
spots are replaced with structured processes, clear accountability, and payer-side expertise. By redesigning the front
end, tightening follow-up discipline, and eliminating bottlenecks in A/R, We were able to help the practice regain control
of its revenue cycle and restore predictable cash flow.
Most importantly, the improvements were not temporary fixes—they created a sustainable operational foundation that
continues to reduce denials, accelerate payments, and support long-term financial stability.
🎯 Want to see what’s possible with your billing process?
Get in touch with us
At Clarity Works AI, we believe every conversation can uncover new opportunities to strengthen your practice’s revenue and simplify your operations. Whether you’re struggling with claim denials, looking to recover lost income, or ready to automate your billing for better results, our team is here to help.
Fill out the form, and one of our team members will reach out to discuss your goals, review your current process, and identify where we can make an immediate impact.
Let’s build a smarter, more predictable financial future for your practice — together.
(407)974-5246
How Can We Help?
Send Us A Message

Innovation
Fresh, creative solutions.

Integrity
Honesty and transparency.

Excellence
Top-notch services.

COMPANY


Copyright 2026. Clarity Works AI. All Rights Reserved.
