From Delays to Dollars: A 60-Day RCM Transformation

The Challenge
Before working with Clarity Works, this multi-provider chiropractic clinic in the Southwest struggled with recurring claim
denials and long reimbursement delays — despite having an experienced in-house billing team.
Each month, payments were stalled due to eligibility errors, missing pre-authorizations, and duplicate claim submissions.
Their billing process had become reactive, consuming valuable staff time and restricting cash flow.
Key Issues:
Front-end verification errors leading to eligibility denials
Lack of pre-authorization tracking for key modalities
Incomplete patient data capture causing clearinghouse rejections
Inefficient denial follow-up processes
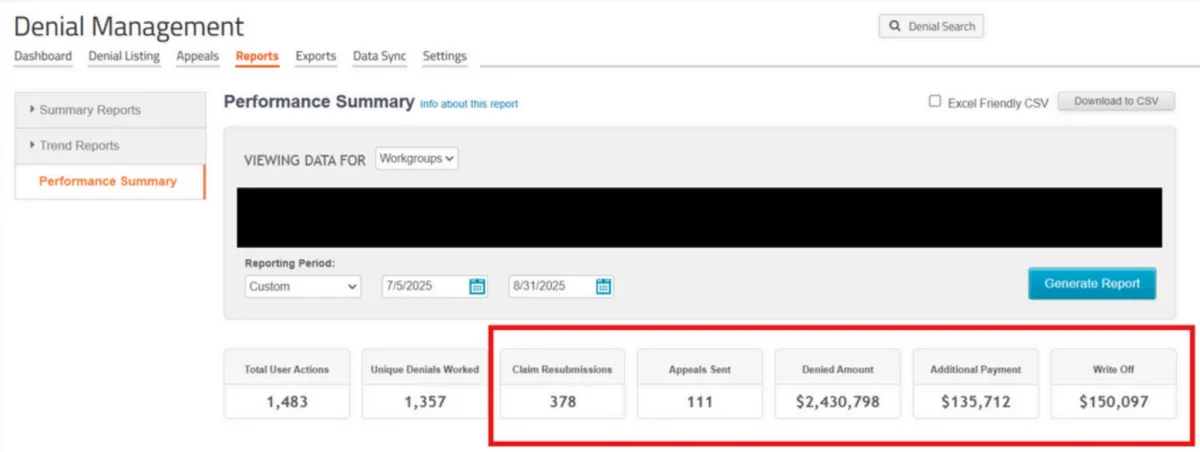
🟥 Starting Point: 378 Claim resubmissions, $2.4M in denied claims
The Solution
We took over full Revenue Cycle Management (RCM) operations under an NDA, implementing a complete five-phase
recovery plan to eliminate rework and restore billing integrity.
1) Insurance Verification & Eligibility Audits (48–72 hrs pre-visit)
Performed pre-visit checks via Availity, UHC Provider Portal, and Aetna Connect; logged deductible status, visit limits,
and plan notes into a shared tracker for the front desk.
Added secondary coverage screening to prevent COB denials and mid-year policy changes from slipping through.
2) Authorization & Coverage Validation (code-level rigor)
Flagged modalities requiring prior auth (e.g., 97035 – Ultrasound, 97110 – Therapeutic Exercise) and submitted pre-auths with supporting documentation through payer portals.
Mapped services to payer-specific rules to avoid downstream denials tied to missing approvals.
3) Claim Scrubbing & Submission Optimization (“perfect-pass” standard)
Instituted hard validation gates so no claims left with clearinghouse or payer-rejectable errors.
Standardized NPI, taxonomy, and diagnosis-linking; enforced modifier prompts for services needing -59 or -XU when billed with manipulative treatments.
Built automation alerts to catch code pairs that typically conflict (e.g., 97140 with 98940–98942).
4) Denial Management & Appeals (payer-specific playbooks)
Deployed templated appeal packets by payer; created a Corrected Claim SOP to reprocess cleanly within timely filing
limits.
Stopped duplicate resubmissions by introducing a single-source protocol for corrected claims and tracking them
through resolution.
5) Reporting & Transparency (operator & exec views)
Weekly reconciliation + A/R aging segmented by payer and CPT helped leadership spot trends early.
Added CPT utilization optimization rules
Common Denial Patterns We Eliminated
Eligibility not verified → dual verification (portal + phone)
Missing modifier (ex: 97140 with manipulation) → real-time modifier alerts.
Non-covered (DX mismatch) → ICD-10↔CPT crosswalk.
Duplicate claim → standardized corrected-claim pathway.
Timely filing → automated deadline tracker
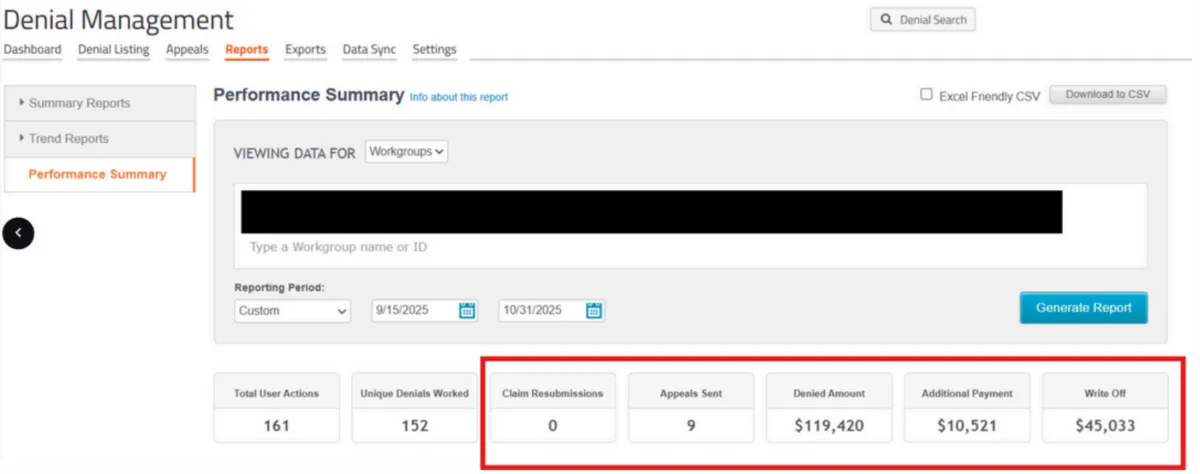
🟩AFTER 60 DAYS: 0 CLAIMS RESUBMITTED,$119,420 LEFT IN DENIED CLAIMS
The Results
The impact was immediate — a 60-day turnaround that redefined the clinic’s billing performance.
Denials reduced by 32% in 60 days through front-end verification, pre-auth discipline, and clean submission rules.
96.8% perfect-pass claim rate achieved by enforcing “no-submit with rejectables” and modifier automation.
A/R days cut from 58 → 29 by eliminating preventable rejections, accelerating corrected claims, and tightening
appeals turnaround.
Monthly reimbursements up 22%, driven by fewer denials, faster first-pass approval, and improved CPT utilization.
Verification accuracy improved across payer types (BCBS, Aetna, UHC, Cigna), reducing eligibility/COB denials and
stabilizing cash flow volatility.
The Takeaway
We turned a chaotic billing cycle into a streamlined, transparent, and data-driven revenue engine.
By focusing on front-end verification, clean submissions, and real-time reporting, the clinic achieved faster payments, higher accuracy, and lasting confidence in its RCM process.
🎯 Want to see what’s recoverable in your billing process?
Get in touch with us
At Clarity Works AI, we believe every conversation can uncover new opportunities to strengthen your practice’s revenue and simplify your operations. Whether you’re struggling with claim denials, looking to recover lost income, or ready to automate your billing for better results, our team is here to help.
Fill out the form, and one of our team members will reach out to discuss your goals, review your current process, and identify where we can make an immediate impact.
Let’s build a smarter, more predictable financial future for your practice — together.
(407)974-5246
How Can We Help?
Send Us A Message

Innovation
Fresh, creative solutions.

Integrity
Honesty and transparency.

Excellence
Top-notch services.

COMPANY


Copyright 2026. Clarity Works AI. All Rights Reserved.
